Cataract Surgery
The described techniques have been approved by many Ophthalmological and Scientific Societies; the text used is recommended by the B.S.C.R.S (Belgian Society of Cataract & Refractive Surgery) in its brochures on Cataract Surgery, a common work of a panel of Ophthalmologists. The B.S.C.R.S. has 220 members, all Ophthalmologists.

Cataracts
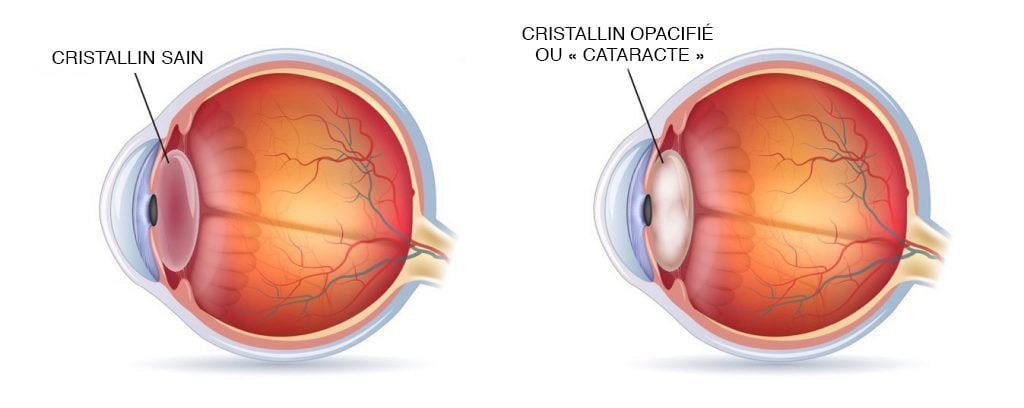
The natural crystalline lens (see Eye) becomes more opaque with time; this is a natural ageing process. Most of the patients being operated on are over 65 years. However, in some patients, the cataract can start earlier than for others; diabetics, high myopes are more at risk of having a cataract earlier; some systemic diseases or the use of drugs (cortison) can play a role.
The main sign of cataract is that the vision diminishes far and / or near; becomes more foggy with time, poorer perception of colors, as well as light aberrations around certain point light sources, can also be observed.and cannot be corrected by glasses anymore.
It is then necessary to undergo a surgical operation.
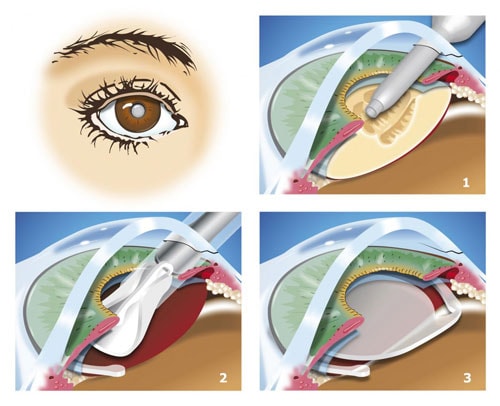
The surgeon, with a small incision of 2.2 to 2.8 mm, will remove (in fact, destroy by ultrasound) the lens that became opaque and replace it by an artificial lens, also called implant.
The procedure is performed under local anesthesia (so-called “topical” anesthesia); only drops are applied to the eye a few minutes before the operation. A small sedative is usually given for the comfort of the patient.
Le signe principal de la cataracte est la diminution d’acuité visuelle, de loin et/ou de près; une moins bonne perception des couleurs, ainsi que des aberrations lumineuses autour de certaines sources lumineuses ponctuelles, peuvent également être observées. Ceci ne peut plus être corrigé par des lunettes; il faudra donc envisager une opération de la cataracte.
Le chirurgien, par une petite incision de 2,2 à 2,8 mm, va ôter (en fait, détruire par ultra-sons) le cristallin devenu opaque et le remplacer par une petite lentille, aussi appelée implant, ou cristallin artificiel.
L’intervention se déroule sous anesthésie locale (dite anesthésie « topique »); uniquement des gouttes sont appliquées dans l’œil quelques minutes avant l’opération. Un petit calmant est généralement donné pour le confort du patient.
For very nervous or anxious patients, a general anesthesia can be used, as well as for special cases, as for example in case of great myopia, etc.
This surgery is performed in ambulatory, that is to say without hospitalization; the patient is allowed to leave the center one hour after the operation. The eye is protected by a protective shield, to avoid any shock. This shield is worn for 24 hours after the operation and then only at night for a week.The day after the operation, the operated eye will be checked at the consultation, to measure the visual acuity and the pressure of the eye; a care sheet with all the explanations concerning the postoperative treatment (antibiotic eye drops and anti-inflammatory eye drops) and the precautions to be taken, is then given to the patient. If necessary, the second eye can be operated fairly quickly after the first one.
The purpose of the surgery is to improve visual acuity, and to allow the patient to function without constantly wearing glasses; however they can be prescribed to further improve the sight, or for reading.
It should be noted that visual recovery is usually rapid after surgery; most patients are able to watch TV on the first day(s).
It is important to remember that the costs of this surgery are not completely covered by I.N.A.M.I. Some of the sterile material is at the patient’s expense, but can be reimbursed by complementary insurance (from the mutual insurance company) or by private insurance.
Artificial Lens
Several implants or artificial lenses exist on the market. The most frequently used implants are soft, pliable, injectable by a small incision.
The power of this implant is calculated during preoperative examinations. It seems more interesting to get a good sight from a distance without glasses (a particular type of implant or toric even allows to correct the astigmatism associated with myopia or hyperopia), and to wear an optical correction for reading. However, some patients may have other wishes.
A new type of artificial crystalline lens has recently been available, making it possible to correct distance vision, but also the near vision, thus allowing reading without glasses.
Studies show that the problems of the past (light aberrations and diminished vision of contrasts) are practically solved in all cases.
However, some patients may need more time than others to get used to these implants.
It is also very important to define beforehand what type of vision (far, near, intermediate for PC) is most useful for each patient, in order to choose the most suitable implant on a case by case basis.
These implants are indicated in very specific cases, depending on the preoperative defect (myopia, hyperopia or astigmatism) and only if they can meet the specific needs of certain patients. They are not reimbursed by the I.N.A.M.I., but can be reimbursed by some private insurance company.
These are brochures published by a commercial company, for the simple purpose of making you understand how this implant work. These brochures were not produced by Dr. Mathys, who assumes no responsibility for their content. They do not replace a consultation with your ophthalmologist.
DO YOU HAVE ANY QUESTIONS?
We will be happy to answer you as soon as possible.